ARTICLE AD BOX

 Getty Images
Getty Images
This month the government in England will launch a consultation for its men's health strategy. The move is long overdue, experts say, with men much more likely to die prematurely than women. But why are they in such poor health – and what can be done about it?
Andrew Harrison was running a men's health clinic from a youth centre in Bradford when he heard a knock. He turned to the door, but no-one was there. Then he heard his name being called. He looked around to see a young man at the window asking for condoms.
"I was on the first floor," he says, recounting the story from a few years ago. "The lad had shimmied up a drainpipe on the outside of the building because he didn't want to go through the reception and ask."
The anecdote, in many ways, encapsulates the challenges over men's health – a combination of risk-taking behaviour and a lack of confidence and skills to engage with health services.
Early deaths
In the UK men are more likely to smoke, drink alcohol, use drugs and have high cholesterol and blood pressure.
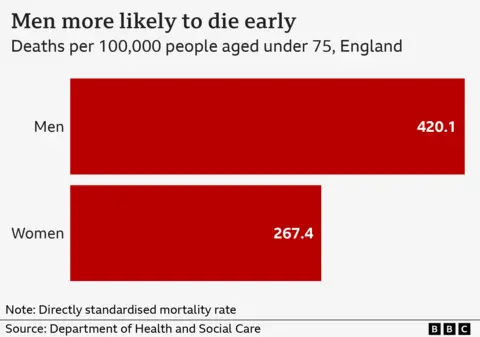
These are major contributors to the fact men have a lower life expectancy than women - by four years - and are nearly 60% more likely to die prematurely before the age of 75 with heart disease, lung cancer, liver disease and in accidents.

Prof Alan White, who founded the Men's Health Forum charity and set up a dedicated men's health centre at Leeds Beckett University, says the issue needs to be taken more seriously.
He cites the pandemic as an example, pointing out that 19,000 more men than women died from Covid. "Where was the outrage? Where was the attention?"
He says it is too easy to blame men's poor health on their lifestyles, arguing "it's much more complex than that."
He says there are biological reasons – the male immune system is less able to fight off infection. But, as the story of the young man seeking condoms above demonstrates, they can also lack the skills to access health services.
Prof White says: "Men are less health-literate, that is to say they don't develop the skills to talk about their health and recognise and act on the signs. Men's health is very static from their teenage years right through into their 40s generally – many go years without see a health professional.
"It is different for women. Getting contraception, having cervical screening and then childbirth means many women have regular contact with health services in a way men do not."
Stark differences
Machismo is also a factor, says Mark Brooks, the policy adviser for the All-Party Parliamentary Group on Men's and Boy's Issues, which has played a key role in influencing the government to draw up a men's health strategy.
"In society we have different expectations in regards to men. They are expected to man up and get on with things, to be strong and resilient."
But he says when it comes to men's health it is important to pay particular attention to the impact of deprivation. Life expectancy in the poorest 10% of areas is 10 years less than in the wealthiest – a larger gap than is seen for women – and in the most deprived areas a man is 3.5 times more likely to die before the age of 75.
"You cannot ignore the stark differences when it comes to left-behind communities and those working in blue-collar jobs like construction and manufacturing," he says. "The way health services are designed isn't working for men."
NHS health checks, which are offered every five years to those aged 40 to 74, are considered a crucial intervention when it comes to many of the diseases which are claiming the lives of men early. But fewer than four in 10 men take up the offer.
"Someone working in construction or on an industrial estate will find it very difficult to take time off whether that's for a health check or to go and see their GP."

 Getty Images
Getty Images
NHS health checks are offered to the over 40s every five years and include blood pressure checks
Mr Brooks says he would like to see employees given a right to two hours' paid time off to go for health checks as well as seeing them delivered in places where blue-collar workers are employed, such as industrial estates.
But he says this is also an issue about employment - with some men in these roles scared to face up to health problems that develop in their 40s and 50s - ignoring early warning signs or hiding illnesses from bosses altogether because of what it may mean for their work.
He adds that job worries and financial concerns, along with relationship problems, are a big driver in the high suicide rates seen among men. Three-quarters of people who take their own lives are men.
Despite this, just a third of people sent for talking therapies are men, which may suggest that services are not doing enough to consider men's needs.
"How services are set up to recognise signs of depression and anxiety is not how men express them – they are more likely to display signs of anger, abuse alcohol or become withdrawn and push people away," says Prof White.
Ethnic differences are also important to recognise, he says. For example, black men in England are twice as likely to be diagnosed with prostate cancer, while men from Indian or Bangladeshi backgrounds are at particularly high risk of diabetes.
Wake-up call
But none of this means men are not interested in their own health, says Prof Paul Galdas, a men's health expert at York University. "Men will open up and want to be engaged, but to do that you have to base it around actions and activities."
He has helped develop a six-week mental fitness programme in partnership with the Movember men's health movement that has been trialled on NHS front-line workers following Covid. Now it is being used by Leeds United football club for its youth players.
Men are provided with support to understand how behaviour affects moods, they are encouraged to track their habits and set goals for healthy activities.
"It can be about going for a walk, seeing friends, playing golf and developing problem-solving skills to protect mental health. Good mental health leads to good physical health."

 Getty Images
Getty Images
Similar activity-based initiatives can be found in a number of local areas where charities, councils and local men's groups have worked together to set up schemes.
The Men's Sheds movement is perhaps the most well-known where men are encouraged to come together and bond and support each other while doing practical projects.
Prof White says now is the time to build on these foundations – something a national men's health strategy is vital for. He says it will help "shine a spotlight" on the issue in a similar way to the women's health strategy did back in 2022 – that led to the creation of a network of women's health hubs and women's health champions at the heart of government.
But he also wants it to act as a "wake-up call" for men themselves. He says there are some simple steps every man should consider.
"Look at your waist size – if you are carrying weight, if your tummy is too big try to do something. Get moving, get out and about and talk to people.
"Take every opportunity to get a health check or screened. And, if you notice changes to body or the way you are managing problems, seek help."

 1 month ago
27
1 month ago
27








 English (US) ·
English (US) ·